ICEECE2012 Poster Presentations Diabetes (248 abstracts)
Protein from Hevea brasiliensis latex rubber tree enhances wound healing in diabetic rats
T. Andrade 1 , G. Caetano 2 , D. Masson 1 , C. Landim 1 , J. Coutinho-Netto 1 , M. Foss 1 & M. Frade 1
University of Sao Paulo, Ribeirao Preto, Brazil.
The healing effects of Hevea brasiliensis latex biomembrane has been widely cited in the literature, mainly regarding its protein fraction F1 in patients with diabetes. The purpose of this study was to evaluate the wound healing mechanism of F1 in diabetic rats. Eighty Wistar rats were used for the experiments, where: 40 rats were induced to diabetes by streptozotocin 45 mg/kg (DM) and 40 rats were left non-diabetic (N). Two wounds were created on the dorsal of each rat using a skin biopsy punch (1.5 mm diameter). The groups were assigned according to treatments: Carboxymethylcellulose (CMC) Gel 4% [DM sham, N sham (n=20)] and CMC +0.01% F1 [(DM F1, N-F1 (n=20)]. Wounds were treated daily, over 21 days. On the 2nd, 7th, 14th and 21st days, animals were euthanized and 10 biopsies/group/day were collected. Wounds reepithelialization was assessed and histological parameters (inflammatory cells, blood vessels, fibroblasts and the percentage of collagen area) were analyzed by HE and Gomori’s trichrome staining. DM-F1 group showed higher reepithelialization rates than DM-sham (p=0.0026) and all wounds were re-epithelialized on the 14th day, different from N-F1 group. In a similar way, DM-F1 group showed higher collagenesis then DM-sham (p=0.0001), different from N-F1; fibroplasia was more evident for DM-F1 (p=0.0001) on the 14th and 21st days. Interestingly, these results can be associated with higher reepithelialization of wounds treated with DM-F1. The metabolic status of diabetes induced chemotaxis of inflammatory cells to the skin, that increased with the injury up to the 7th day (p=0.0026), mainly when wounds were treated with DM-F1. Angiogenesis was more pronounced for DM-F1 group on the 7th an 14th days. The inflammatory process triggered by the metabolic stress of diabetes mellitus seemed to add and interact with the stimulus induced by F1, accelerating the cutaneous wound healing when compared to non-diabetic groups.
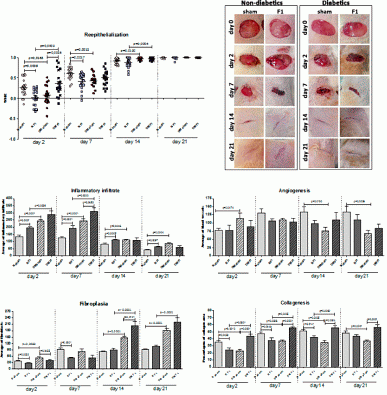
Distribution of variables reepithelialization by Wound Healing Rate (WHR), inflammatory infiltrate, angiogenesis, fibroplasia and collagenesis of wounds treated topically with F1 (F1 groups) and non-treated (sham groups) in non-diabetic (N-F1 ou N-sham) and diabetic (DM-F1 or DM-sham) rats, for 2, 7, 14 and 21 days of follow-up.
Declaration of interest: The authors declare that there is no conflict of interest that could be perceived as prejudicing the impartiality of the research project.
Funding: This work was supported, however funding details unavailable.




