ECE2011 Poster Presentations Thyroid (non cancer) (78 abstracts)
Occurrence and prognostic impact of hypothyroidism in chronic heart failure
V Triggiani 1 , M Iacoviello 2 , F Monzani 3 , V A Giagulli 1 , E Tafaro 1 , P Guida 2 , E Guastamacchia 1 & S Favale 2
1Endocrinology and Metabolic Diseases, University of Bari, Bari, Italy; 2Cardiology, University of Bari, Bari, Italy; 3Internal Medicine, University of Pisa, Pisa, Italy.
The aim of this study was to define the occurrence of hypothyroidism and its impact on CHF progression. Four hundred and twenty-two consecutive outpatients (326 males, aged 65±12 years) with CHF in stable condition and conventional therapy were evaluated. Thyroid status was checked at least every 4 months. The progression of heart failure was defined as death, urgent heart transplantation, or hospitalisation due to worsening HF.
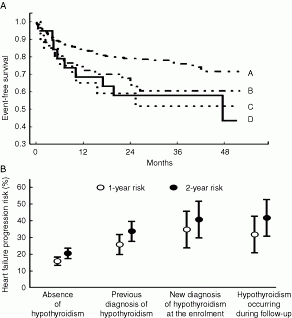
Figure 1 (A) Heart failure progression in subgroups with euthyroid status at the enrolment and during follow-up (Group A), previous diagnosis of hypothyroidism (Group B), new diagnosis of hypothyroidism at the enrolment (Group C) and occurrence of hypothyroidism during follow-up (Group D). (B) Probability of 1- and 2-year occurrence of heart failure progression in different subgroups.
Results: A total of 51 patients (12%) had a previous diagnosis of hypothyroidism while 21 (5%) were newly diagnosed at the enrolment (prevalence of hypothyroidism at the first evaluation: 17%; 33% in females vs 13% in males; P<0.001). During follow-up (median 28 months) hypothyroidism occurred in further 19 patients (incidence rate: 26/1000/year) and it was mainly attributable to amiodarone therapy. In patients affected by hypothyroidism a significantly greater occurrence of heart failure progression was observed (Fig. 1A/B).
 }
}



