SFEBES2012 Poster Presentations Clinical practice/governance and case reports (90 abstracts)
A rare case of prolactinoma presenting with psychosis
Ruth Witherall , Helena Gleeson , Trevor Howlett & Miles Levy
Department of Endocrinology, University Hospitals of Leicester, Leicester, United Kingdom.
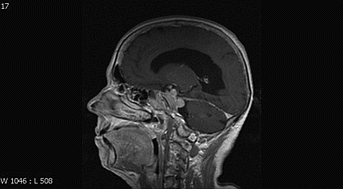
Case History: An 84-year-old women presented to a psychiatric unit with a 5-month history of fluctuating confusion, paranoid behaviour, anxiety, reduced cognition and unsteadiness. There was no history of galactorrhoea, headache or visual field disturbance. Past medical history included hypertension, chronic kidney disease, congestive heart failure, premature menopause and hyperlipidaemia. She had been taking bendroflumethiazide, furosemide, mirtazepine and sulpiride. A CT head demonstrated a large mass in the pituitary fossa, and MRI confirmed a large pituitary lesion with suprasellar extension and cavernous sinus invasion causing hydrocephalus due to compression of the aqueduct. Serum prolactin after dilution measured >400,000 miU/l and a diagnosis of macroprolactinoma was made. She was started on cabergoline and made an excellent response. Her sulpiride was discontinued in favour of quetiapine and within six months her prolactin was suppressed and the suprasellar extension and dilated ventricles had improved. Within one year her psychiatric symptoms and cognitive decline had completely resolved, her psychotropic medications were stopped and she was living independently.
Discussion: This is a rare presentation of macroprolactinoma causing hydrocephalus and secondary psychiatric symptoms resolving promptly after dopamine agonist therapy. We have previously described two cases of macroprolactinoma presenting with neurological symptoms due to hydrocephalus (1). This case demonstrates the importance of considering the diagnosis of prolactinoma in patients despite being on dopamine antagonist therapy; the very high level of prolactin and scan appearances were consistent with macroprolactinoma rather than drug-induced hyperprolactinaemia. Because quetiapine is not a D2 receptor antagonist, the change from sulpiride may have facilitated the rapid biochemical and radiological response to cabergoline. This case raises several interesting aspects of prolactinoma management including the atypical presentation, the association with hydrocephalus, and the pharmacological considerations both in diagnosis and treatment. (1) Khan EG, Howlett TA. (1995) Two macroprolactinomas presenting with neurological signs. J RSM 88: 111P–112P.
Declaration of interest: There is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
Funding: No specific grant from any funding agency in the public, commercial or not-for-profit sector.