SFEBES2012 Poster Presentations Neoplasia, cancer and late effects (17 abstracts)
Metastatic medullary thyroid carcinoma causing Cushing’s syndrome
Leena Krishnan , Vidya Srinivas , Firas Hadaddin & Francesca Swords
Diabetes and Endocrinology, NNUH, Norwich, United Kingdom.
A 26 year old lady presented with a 4/12 history of abdominal distension and lethargy. PMH included learning difficulties and congenital hypotonia and she was in long-term foster care.Diabetes had been diagnosed requiring insulin a few months previously. Examination revealed her to be extremely unwell, with proximal myopathy, purple striae, hirsutism and a firm nodular thyroid gland. She was hypokalaemic (2.8 mmol/l) and alkalotic. Cushing’s assessment(table) revealed ACTH dependent Cushing’s. CT scan of the pituitary was normal, abdomen confirmed bilaterally bulky adrenals and neck and chest confirmed the presence of lymphadenopathy and a grossly abnormal thyroid. US FNA of her neck lymph node confirmed medullary thyroid cancer, and a presumptive diagnosis of MEN2b was made as evidenced by mucosal neuromas over the tongue, and metastatic medullary thyroid cancer secreting ACTH leading to Cushing’s syndrome. She was started on metyrapone and was immediately able to stop insulin. Unfortunately, she then deteriorated and was transferred to HDU for monitoring, central potassium infusions and consideration of an etomidate infusion. Despite high dose metyrapone, serum cortisol levels remained elevated >1000 nmol/l. Ketoconazole was therefore added and her condition improved further. Several days following HDU discharge, she became unwell again and glucocorticoid insufficiency was suspected, so a block and replace regimen was instituted (with dexamethasone). Subsequent outpatient octreotide and MIBG scans revealed abnormal tracer uptake limited to the root of the neck and upper mediastinum. She continued to improve as an outpatient, has now undergone bilateral adrenalectomy, and is currently well on replacement therapy. We felt her Cushing’s was life threatening, so its definitive treatment took priority over the medullary thyroid cancer. However, total thyroidectomy and lymph node dissection is now planned.
Declaration of interest: There is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
Funding: No specific grant from any funding agency in the public, commercial or not-for-profit sector.
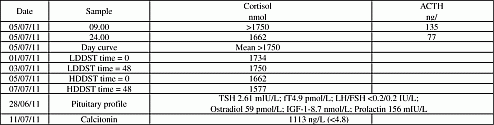
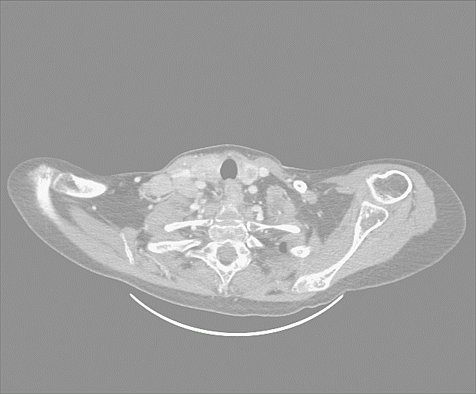
Enlarged thyroid with adjacent lymphadenopathy

 }
}



