SFEBES2012 Poster Presentations Clinical practice/governance and case reports (90 abstracts)
We should “ruddy well follow them up” - An unusual complication of suboptimally treated Congenital Adrenal Hyperplasia
Pallai Rappai Shillo , Ruth Macinerney & Robert Robinson
Endocrinology, Chesterfield Royal Hospital, Chesterfield, United Kingdom.
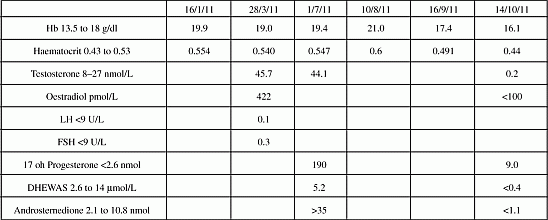
A 40 year old man with CAH and significant needle phobia presented with left leg pain in January 2011. He had been discharged from follow up at another trust. Medications were hydrocortisone 10 mg BD and fludrocortisone 100 mcg OD. Admission haemoglobin was 19.9 g/dl, haematocrit 0.554. A thorough work up to investigate causes of polycythaemia revealed the only significant abnormality as a testosterone of 45.7 nmol/L (8–27), with low gonadotrophins. The blood sample for 17-OHP and adrenal androgens was lost; he had venesection on initial admission but was reluctant to return. He denied lack of concordance. When he agreed repeat testing 17 OH progesterone and adrenal androgens confirmed under replacement with glucocorticoid resulting in high testosterone and adrenal androgens. Hydrocortisone was stopped and dexamethasone 1mg nocte started resulting in suppression of adrenal androgens and exposing secondary hypogonadism due to gonadotrophin suppression from adrenal testosterone. Investigations See table below Conclusion We describe polycythaemia due to androgen excess in a man with suboptimally treated CAH. Androgen excess leads to polycythaemia via stimulation of erythropoiesis, and although this is documented, androgenic polycythaemia in CAH has rarely been reported. Our patient’s case highlights the dangers of androgen excess in CAH, and is a reminder of why such patients should remain under the care of endocrinologists.
Declaration of interest: There is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
Funding: No specific grant from any funding agency in the public, commercial or not-for-profit sector.
Investigations Venesection (18/1/11 & 17/8/11) Dex1mg ON from 19/7/11
 }
}



