SFEBES2012 Poster Presentations Clinical practice/governance and case reports (90 abstracts)
Transient thyrotoxicosis following parathyroidectomy
Biju Jose 1 , Tarek Hiwot 2 , Nicholas Inston 2 , Andrew Ready 2 & Neil Gittoes 1
1Department of Endocrinology, University hospital birmingham, Birmingham, United Kingdom; 2Department of Renal surgery, University hospital birmingham, Birmingham, United Kingdom.
Introduction: Thyrotoxicosis of iatrogenic origin is well recognized, particularly with use of drugs such as amiodarone and lithium. However, thyrotoxicosis after parathyroid surgery is rarely reported and has been poorly characterized within prospective studies. We report the case of a lady who underwent parathyroidectomy who developed self-limiting thyrotoxicosis.
Case: A 42 year old lady presented with recurrent urinary tract infections due to bilateral staghorn calculi. She was found to have primary hyperparathyroidism and underwent an uncomplicated open parathyroidectomy with resultant normalisation of serum calcium and parathyroid hormone levels. The histopathology was consistent with an adenomatoid, hyperplastic nodule of the right parathyroid gland with no evidence of malignancy. One week post-operatively she developed profuse sweats, tremor, dyspnoea and anxiety. Clinically she was thyrotoxic. Thyroid function tests confirmed the clinical suspicion (Table 1). She was recommended to start carbimazole 20 mg daily, but following interrogation of the internet, the patient decided to withhold any active treatment, assuming that her thyrotoxic state was related to recent parathyroidectomy. She was reviewed in 4 weeks, by which time her symptoms and signs had abated and repeat thyroid function, calcium and parathyroid levels were normal (Table 1). Anti thyroperoxidase antibody titres were undetectable.
Discussion: This case demonstrates the development of transient thyrotoxicosis after exploration of the neck during parathyroid surgery. It is a poorly characterized and rarely diagnosed phenomenon. Physical trauma to the thyroid gland during exploration may result in a transient thyroiditis, which is usually self-limiting but may require symptomatic treatment. This case highlights the importance of being aware of this potential consequence of parathyroid exploration and the need for a considered approach to management as anti-thyroid medication is unlikely to be either necessary or of clinical value.
Declaration of interest: There is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
Funding: No specific grant from any funding agency in the public, commercial or not-for-profit sector.
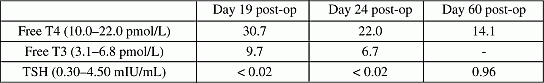
Table 1: Thyroid function tests following surgery
 }
}



