SFEBES2012 Poster Presentations Clinical practice/governance and case reports (90 abstracts)
An Unusual Clinical Presentation May Indicate an Unusual Condition: Phaeochromocytoma presenting as Acute Left Ventricular Failure
Christian Hariman 1,2 , David Jenkins 1 & Paul Newrick 1
1Diabetes & Endocrinology, Worcester Royal Hospital, Worcester, United Kingdom; 2Diabetes & Endocrinology, Univeristy Hospital Coventry & Warwickshire, Coventry, United Kingdom.
Introduction: Acute left ventricular failure is rarely caused by phaeochromocytoma. The rarity and severity of this presentation may result in delayed investigation and incorrect management.
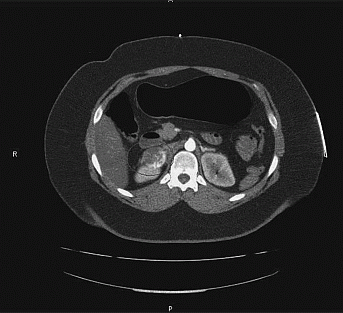
Case Report: A 22 year old woman was admitted with headache, vomiting, back pain and malaise. She was initially treated for suspected septic shock with intravenous antibiotics and fluids. Within 24 hours of admission, she rapidly deteriorated and developed pulmonary oedema and cardiogenic shock which required a one-week ITU admission and inotropic support. Her echocardiogram showed an akinetic mid to apical left ventricle, and she initially underwent treatment and investigations for acute myocarditis. Phaeochromocytoma was eventually diagnosed 8 days after admission based upon her history and a 4cm right adrenal tumour found on her urgent CT imaging. The diagnosis was further confirmed by raised plasma metanephrines and elevated urinary catecholamine metabolites. She subsequently made a good recovery following initial stabilisation with Phenoxybenzamine. After 3 months of continued alpha and subsequent beta-blockade she underwent a successful right adrenalectomy.
Conclusion: The rarity of both phaeochromocytoma and pulmonary oedema in a young patient resulted in incorrect initial management. Although rare, phaeochromocytoma should be considered in unexplained acute pulmonary oedema in a young patient. Early alpha-blockade should be carefully considered if the index of suspicion is high.
Declaration of interest: There is no conflict of interest that could be perceived as prejudicing the impartiality of the research reported.
Funding: No specific grant from any funding agency in the public, commercial or not-for-profit sector.
 }
}



