ICEECE2012 Poster Presentations Pituitary Clinical (183 abstracts)
Diabetes insipidus could be the initial sign of primary hypophysitis
S. Suh, S. Park, J. Joung, Y. Cho, S. Jin, S. Kim, H. Kim, J. Bae, J. Kim, S. Kim, J. Chung, Y. Min, M. Lee, M. Lee & K. Kim
Samsung Medical Center, Seoul, Republic of Korea.
Introduction: The natural history of primary hypophysitis is incompletely understood and best treatment remains controversial.
Methods: We performed a retrospective study of 19 patients (mean age of 47 years, fifteen women and four men) who were diagnosed with primary hypophysitis in Samsung Medical Center in Seoul, Korea, from January 2001 to October 2011.
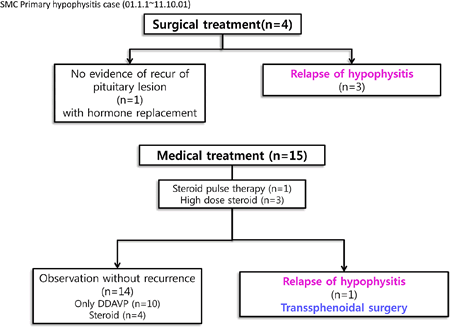
Results: Two patients had recent pregnancy and underlying autoimmunity. Most common clinical feature was polyuria and polydipsia (78%) and most common endocrinological finding was also diabetes insipidus (DI, 73%). The initial presumptive diagnosis was pituitary adenoma or lymphoma in eight patients (42%) and inflammatory hypophysitis in eleven (57%). The first eight patients underwent transsphenoidal surgery but only four (21%) proceeded to total tumor removal. Four patients (21%) received steroid therapy of whom one patient relapsed with pressure symptoms and later underwent surgery. Half of the patients under steroid treatment suffered from side effects such as facial swelling and body weight gain. Only one patient (25%) did not respond satisfactorily to steroid therapy and later underwent surgery. Altogether, the histological diagnoses were confirmed in nine patients, seven lymphocytic hypophysitis (77%), each one of granulomatous and xanthomatous hypophysitis (11% respectively). All patients who underwent surgery required long-term hormone replacement, three (75%) relapsed and needed additional radiotherapy or steroid therapy. Eleven (57%) patients who had no pressure or visual symptoms received only conservative management with hormone replacement (i.e. vasopressin for DI). All these eleven patients have been regularly followed up without recurrence.
Conclusion: Diabetes insipidus could be the initial sign of primary hypophysitis and controlled satisfactorily without aggressive treatment.
Follow-up status of patients with primary hypophysitis.
Declaration of interest: The authors declare that there is no conflict of interest that could be perceived as prejudicing the impartiality of the research project.
Funding: This research did not receive any specific grant from any funding agency in the public, commercial or not-for-profit sector.
 }
}



