UKINETS2016 Oral Communications (1) (3 abstracts)
Tumour size is not a reliable criterion for management of patients with Non-secreting pancreatic neuroendocrine tumours: results of a large, multi-centre, operative cohort
Logan Mills 1 , Panagiotis Drymousis 2 , J Vashist 3 , C Burdelski 3 , Andreas Prachalias 1 , Parthi Srinivasan 1 , Krishna Menon 1 , Saboor Khan 4 , Judith Cave 5 , Thomas Armstrong 5 , MO Weickert 4 , Andreja Frilling 2 , JK Ramage 1 & Raj Srirajaskanthan 1
1King’s College Hospital, London, UK; 2Imperial College, London, UK; 3University Hospital, Hamburg, Germany; 4University Hospitals Coventry and Warwickshire, Coventry, UK; 5University Hospital, Southampton, UK.
Background: Small pancreatic neuroendocrine tumours (PNETs) present a management dilemma because of their uncertain natural history. Some clinicians believe that lesions <2 cm are indolent and can be managed with surveillance. By contrast, the most recent WHO classification system regards all PNETs as potentially malignant.
Aim: To assess the malignant behaviour of small PNETs in a large, retrospective, multicentre patient cohort.
Methods: Patients were retrospectively identified from 5 hospitals using inclusion criteria of non-functional, non-familial, resected PNETs of all stages and grades. Logistic regression for clinical, biochemical and pathological variables, and cox regression for survival data, were performed using SPSSv22.
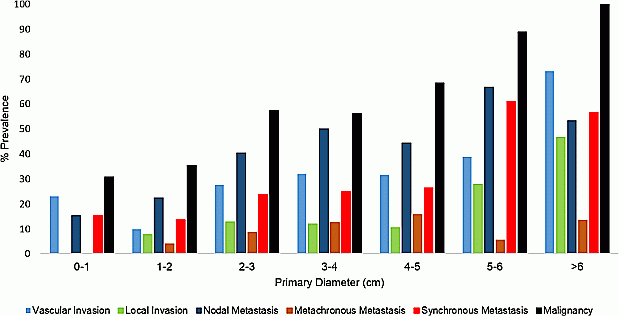
Results: 216 patients with a resected PNET were identified. 64 (30%) had tumours ≤2 cm. Surgical procedures included 80 Whipple’s resections, 124 distal pancreatectomies, 7 enucleations and 2 total pancreatectomies. Malignancy was defined as any of local, vascular or lymphatic invasion or distant metastasis. Overall, malignancy was confirmed in 134 (62%) patients; 22 (34%) tumours ≤2 cm were malignant, compared to 112 (74%) >2 cm. (Figure 1) Tumours ≤2 cm were staged as stage I:38, II:5, III:11 IV:10. The smallest primary with nodal metastasis was 6 mm and with liver metastasis, 10 mm. Prediction of malignancy was not possible in tumours ≤2 cm as logistic regression revealed no association between malignancy and diameter, symptomatic presentation, Ki67 or CgA.
The median survival of this entire cohort was 202 months. 3-year survival did not differ across the 2 cm threshold (≤2 cm 87.0%, >2 cm 80.3%, P=0.151). Significant prognostic factors for the whole cohort included age (hazard ratio 1.07, P=0.04), diameter (HR 1.01, P=0.018), positive nodes (HR 2.041, P=0.026), TNM stage (P<0.05), extrahepatic disease (HR 2.42, P=0.019) and grade (G1 HR 0.11, P<0.001; G2 HR 0.33, P=0.003). Interestingly, surgical margin involvement and extent of nodal positivity (e.g. 2/27) were not prognostically significant. Subgroup analysis of tumours ≤2 cm showed that diameter was not prognostically significant (P=0.15).
Conclusions: 1) 34% of PNETs ≤2 cm displayed malignant features.
2) Metastatic disease was reported in primaries as small as 6 mm, therefore making diameter based surveillance problematic.
3) 3-year survival was not significantly better for tumours ≤2 cm than for tumours >2 cm, reflecting the malignant potential shared by all PNETs.
 }
}



