UKINETS2016 Poster Presentations (1) (35 abstracts)
Initial experience of a novel technique for endoscopic full thickness resection of rectal neuroendocrine tumours
Michelle Fong 1 , Emma Ramsey 1 , Philip Boger 1 , Praful Patel 1 , Richard Ellis 2 & John Knight 1
1Wessex Neuroendocrine Tumour Group, University Hospital Southampton, Southampton, UK; 2Wessex Neuroendocrine Tumour Group, Portsmouth Hospitals NHS Trust, Portsmouth, UK.
Introduction: Standard endoscopic resection of rectal neuroendocrine tumours (NETs) is often associated with histological incomplete excision due to the submucosal position of the tumour within the bowel. This can lead to multiple attempts to achieve a complete excision or uncertainty leading to ongoing endoscopic surveillance. Endoscopic full thickness resection may allow early definitive management. We report a simple definitive technique for the full thickness excision of rectal NETs using a novel endoscopic full thickness resection device (FTRD).
Methods: All patients who presented to the regional NET multidisciplinary team (MDT) meeting with a histologically confirmed rectal NET between January 2015 and August 2016 were included. Electronic records of endoscopy and histology reports, as well as MDT discussions were identified and prospectively analysed. The procedure was undertaken using an over-the-scope FTRD.
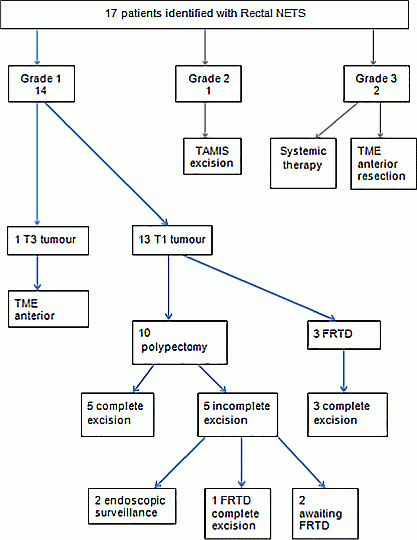
Results: Seventeen patients were identified, 9 male with median age 55 years. A rectal NET was identified at routine bowel screening (7); endoscopic investigation of rectal bleeding (4) and diarrhoea (3); colorectal cancer surveillance (1) and unrecorded in (2) patients. There were 14 grade1 NETs: 13 T1 tumours underwent endoscopic treatment and 1 T3 tumour had surgery. Of those 13 patients, 10 had initial polypectomy with an incomplete excision in 5 patients. 1 patient went on to have FTRD of the scar which confirmed complete excision and 2 further patients are awaiting FTRD. The 3 remaining patients underwent initial FTRD, all with complete excision although the deep excision margin was <1 mm in all. There were no FTRD related complications such as bleeding or perforation. Of the remaining 3 patients, one was grade 2 and underwent TAMIS surgical excision and two were grade 3; one had surgical resection and the other had systemic treatment for metastatic disease.
Conclusion: Full thickness endoscopic resection with FTRD is a promising technique, offering a simple and safe method for obtaining or confirming complete excision of the tumour. The close deep resection margins achieved even with this technique highlight the difficulties in obtaining a deep resection in order to confirm adequate local treatment. Further data are needed to confirm its position in the management algorithm of rectal NETs.
 }
}



