ECE2019 Poster Presentations Thyroid 3 (74 abstracts)
Coexistence of primary mucosa-associated lymphoid tissue lymphoma of thyroid and papillary thyroid microcarcinoma in a background of hashimoto’s thyroiditis
Hakan Duger , Murat Calapkulu , Bekir Ucan , Erman Cakal , Mustafa Özbek & Demet Yılmazer
Ankara Yıldırım Beyazıt Dışkapı Training and Research Hospital, Ankara, Turkey.
Introduction: Papillary thyroid carcinoma (PTC) is the most common endocrine cancer however extranodal marginal zone lymphoma of the mucosa-associated lymphoid tissue (MALT) of the thyroid gland is quite rare. The simultaneous association of both cancers is much more rare.
Case report: 65-year-old woman underwent a thyroid ultrasound examination due to palpable thyroid nodules. Thyroid ultrasound revealed thyroiditis and multiple nodules on the right and left sides. The results of routine laboratory tests were normal and serum hormone measurements showed a thyroid-stimulating hormone (TSH) value of 1.80 mU/l (reference range 0.27–4.2), free T4 value of 0.85 ng/dl (reference range 0.58–1.6), thyroglobulin antibodies of 133 IU/ml (reference range 0–4), and peroxidase autoantibody of 1.3 IU/ml (reference range 0–9). Although the biopsies were benign, total thyroidectomy was performed due to the presence of multiple nodules and therefore with the concern that the subsequent follow-up would be difficult. Histopathology examination revealed a papillary thyroid microcarcinomas in the right lobe was 0.45 cm and in the left lobe 0.6 cm in diameter a predominant follicular pattern (Figure 1A) accompanied with MALT lymphoma showing transformations to diffuse large B-cell lymphoma (Figure 1B and 1C). She reported no systemic B symptoms related to lymphomas. The staging procedures with contrast enhanced computed tomography of neck, thorax and abdomen revealed no evidence of metastasis but bone marrow biopsy was consistent with marginal zone lymphoma metastasis. Thyroid tissue or pathological lymph node was not detected in post-operative 3rd month ultrasound.
Conclusion: Herein, we presented a case with concomitance of thyroid papillary microcarcinoma and MALT in a background of hashimoto’s thyroiditis. In contrast to published cases and despite transformation to DLBCL our patient was asymptomatic. The prognosis of the extranodal marginal zone lymphoma of MALT localized to the thyroid is excellent; however, its known that patients with extrathyroidal invasion or transformation to high-grade lymphoma have poor prognosis. As a result, extranodal marginal zone lymphoma of the thyroid gland is rare and its pathogenesis is not fully understood. Despite the rarity of PTL, it can simultaneously exist with PTC, especially in patients with Hashimoto thyroiditis and the treatment has to prioritize the tumor with worse stage and condition.
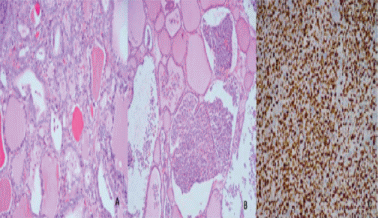
Figure 1 (A) Hematoxylin-eosin staining showing follicular variant papillary microcarcinoma (200 x magnification) (B) lymphoid infiltrate filling the follicle lumen (100 x magnification) and (C) Ki-67 proliferation index of the tumor was 90% (200 x magnification)



