ECE2013 Oral Communications Thyroid (6 abstracts)
Subclinical hyperthyroidism and risk of cardiovascular and all-cause mortality
Christian Selmer 1, , Jonas Olesen 1 , Jesper Madsen 2 , Jens Faber 3 , Peter Hansen 1 , Ole Pedersen 4 , Morten Hansen 1 , Christian Torp-Pedersen 6 & Gunnar Gislason 1
1Department of Cardiology, Gentofte University Hospital, Hellerup, Denmark; 2Copenhagen General Practitioners Laboratory, Copenhagen, Denmark; 3Department of Endocrinology, Herlev University Hospital, Herlev, Denmark; 4Department of Cardiology, Roskilde University Hospital, Roskilde, Denmark; 5Department of Cardiology, Herlev University Hospital, Herlev, Denmark; 6Institute of Health, Science and Technology, Aalborg University, Aalborg, Denmark.
ESE Young Investigator Award
Background: It is still discussed if subclinical hyperthyroidism and ‘high-normal’ thyroid function are risk-factors for cardiovascular mortality.
Objectives: To examine the risk of cardiovascular and all-cause mortality in relation to subclinical hyperthyroidism.
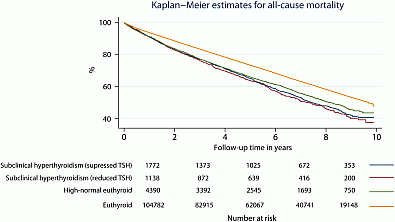
Methods: Patients consulting their general practitioner from 2000 to 2009 in Copenhagen, Denmark, who underwent thyroid blood tests, were identified by individual-level linkage of nationwide registries. Patients with a history of thyroid disease or related medication were excluded. Risk of cardiovascular mortality was analyzed using Kaplan–Meier curves and Poisson regression models were applied to estimate Incidence Rate Ratios (IRR).
Results: Of 574 595 included individuals (mean age 48.7 years (S.D. ±18.3); 39.1% males) 550 927 (95.9%) were euthyroid, 1603 (0.3%) had overt hypothyroidism, 11 834 (2.1%) subclinical hypothyroidism, 3967 (0.7%) overt hyperthyroidism and 6264 (1.1%) subclinical hyperthyroidism. Increased risk of cardiovascular mortality was found in two levels of subclinical hyperthyroidism (TSH <0.1, 0.1–0.2 mU/l and normal free thyroixine): IRR 1.24 (95% CI: 1.09–1.41), IRR 1.21 (1.09–1.34) and in ‘high-normal’ levels of euthyroidism (TSH 0.2–0.4 mU/l): IRR 1.21 (1.13–1.29).
Conclusions: Subclinical hyperthyroidism and ‘high-normal’ thyroid function are significant risk-factors for cardiovascular and all-cause mortality.
 }
}



